Warburg, Otto_Prime Cause of Cancer
By now, you may have heard about the amazing potential health benefits of fasting. While many believe it’s an unhealthy and even dangerous practice, the science says otherwise. Even intermittent fasting, which involves restricting your eating time to an 8-10 hour window rather than going without food entirely, has proven to have many health benefits.
Think about it this way: Our early ancestors did not always have access to food. We ate when we had food and fasted (if involuntarily) when we didn’t. And it’s the same with animals in the wild. They aren’t eating breakfast, lunch, and dinner every single day; they will gorge themselves when they catch some prey, but then often go long periods of time in between each catch.
Indeed, studies have shown that fasting for just three days can not only boost your immune system, but regenerate it entirely, helping to ensure a long and healthy life. The researchers who conducted the study described it as remarkable and a major breakthrough — no kidding! This study showcases how starving the body actually kickstarts stem cells into producing new white blood cells, which will then fight off infection.
Beneficial for Cancer Patients
Fasting for 72 hours will also help protect cancer patients from the toxicity of chemotherapy. Chemo can be quite taxing on the immune system, but the results of this study suggest that fasting can help to alleviate some of the harmful effects that come along with chemotherapy treatment.
In fact, researchers suggest that fasting flips a regenerative switch. How amazing is that? Fasting is something that, with a little research, anyone can easily do. Better still, it costs nothing!
Professor Valter Longo, lead researcher of the study and a professor of both gerontology and biological sciences at the University of California, said the study proved that fasting can, in fact, assist the body with producing a new immune system. As Longo explains:
It gives the OK for stem cells to go ahead and begin proliferating and rebuild the entire system. And the good news is that the body got rid of the parts of the system that might be damaged or old, the inefficient parts, during the fasting. Now, if you start with a system heavily damaged by chemotherapy or aging, fasting cycles can generate, literally, a new immune system.
For the study, participants were asked to fast regularly for periods of two to four days over a six month period. Along with a regenerated immune system, researchers also observed reduced levels of IGF-1, a growth-factor hormone linked to aging, tumour progression, and cancer risk.
According to Longo, the researchers were actually surprised when they realized the outcome of the experiment: “What we started noticing in both our human work and animal work is that white blood cell count goes down with prolonged fasting. Then when you re-feed, the blood cells come back. So we started thinking, well, where does it come from?”
Prolonged fasting not only forces the body to get energy from its own stores of glucose and fat, but it also breaks down a large portion of white blood cells. During each fast cycle the depletion of white blood cells triggers stem cell based regeneration of new immune system cells.
“We could not predict that prolonged fasting would have such a remarkable effect in promoting stem cell-based regeneration of the hematopoietic system,” Longo says. “When you starve, the system tries to save energy, and one of the things it can do to save energy is to recycle a lot of the immune cells that are not needed, especially those that may be damaged”
If the practice of fasting resonates with you, please do your research before trying this yourself. There are tons of resources available online, and many religions and cultures around the world have promoted fasting as the key to optimal health for thousands of years. This could be just the thing you need to kickstart your immune system and give your digestive system a break.
In the first evidence of a natural intervention triggering stem cell-based regeneration of an organ or system, a study in the June 5 issue of the Cell Stem Cell shows that cycles of prolonged fasting not only protect against immune system damage — a major side effect of chemotherapy — but also induce immune system regeneration, shifting stem cells from a dormant state to a state of self-renewal.
In both mice and a Phase 1 human clinical trial involving patients receiving chemotherapy, long periods of not eating significantly lowered white blood cell counts. In mice, fasting cycles then “flipped a regenerative switch,” changing the signaling pathways for hematopoietic stem cells, which are responsible for the generation of blood and immune systems, the research showed.
The study has major implications for healthier aging, in which immune system decline contributes to increased susceptibility to disease as people age. By outlining how prolonged fasting cycles — periods of no food for two to four days at a time over the course of six months — kill older and damaged immune cells and generate new ones, the research also has implications for chemotherapy tolerance and for those with a wide range of immune system deficiencies, including autoimmunity disorders.
“We could not predict that prolonged fasting would have such a remarkable effect in promoting stem cell-based regeneration of the hematopoietic system,” said corresponding author Valter Longo, Edna M. Jones Professor of Gerontology and the Biological Sciences at the USC Davis School of Gerontology and director of the USC Longevity Institute. Longo has a joint appointment at the USC Dornsife College of Letters, Arts and Sciences.
“When you starve, the system tries to save energy, and one of the things it can do to save energy is to recycle a lot of the immune cells that are not needed, especially those that may be damaged,” Longo said. “What we started noticing in both our human work and animal work is that the white blood cell count goes down with prolonged fasting. Then when you re-feed, the blood cells come back. So we started thinking, well, where does it come from?”
Prolonged fasting forces the body to use stores of glucose, fat and ketones, but it also breaks down a significant portion of white blood cells. Longo likens the effect to lightening a plane of excess cargo.
During each cycle of fasting, this depletion of white blood cells induces changes that trigger stem cell-based regeneration of new immune system cells. In particular, prolonged fasting reduced the enzyme PKA, an effect previously discovered by the Longo team to extend longevity in simple organisms and which has been linked in other research to the regulation of stem cell self-renewal and pluripotency — that is, the potential for one cell to develop into many different cell types. Prolonged fasting also lowered levels of IGF-1, a growth-factor hormone that Longo and others have linked to aging, tumor progression and cancer risk.
“PKA is the key gene that needs to shut down in order for these stem cells to switch into regenerative mode. It gives the OK for stem cells to go ahead and begin proliferating and rebuild the entire system,” explained Longo, noting the potential of clinical applications that mimic the effects of prolonged fasting to rejuvenate the immune system. “And the good news is that the body got rid of the parts of the system that might be damaged or old, the inefficient parts, during the fasting. Now, if you start with a system heavily damaged by chemotherapy or aging, fasting cycles can generate, literally, a new immune system.”
Prolonged fasting also protected against toxicity in a pilot clinical trial in which a small group of patients fasted for a 72-hour period prior to chemotherapy, extending Longo’s influential past research.
“While chemotherapy saves lives, it causes significant collateral damage to the immune system. The results of this study suggest that fasting may mitigate some of the harmful effects of chemotherapy,” said co-author Tanya Dorff, assistant professor of clinical medicine at the USC Norris Comprehensive Cancer Center and Hospital. “More clinical studies are needed, and any such dietary intervention should be undertaken only under the guidance of a physician.”
“We are investigating the possibility that these effects are applicable to many different systems and organs, not just the immune system,” said Longo, whose lab is in the process of conducting further research on controlled dietary interventions and stem cell regeneration in both animal and clinical studies.
The study was supported by the National Institute of Aging of the National Institutes of Health (grant numbers AG20642, AG025135, P01AG34906). The clinical trial was supported by the V Foundation and the National Cancer Institute of the National Institutes of Health (P30CA014089).
Chia Wei-Cheng of USC Davis was first author of the study. Gregor Adams, Xiaoying Zhou and Ben Lam of the Eli and Edythe Broad Center for Regenerative Medicine and Stem Cell Research at USC; Laura Perin and Stefano Da Sacco of the Saban Research Institute at Children’s Hospital Los Angeles; Min Wei of USC Davis; Mario Mirisola of the University of Palermo; Dorff and David Quinn of the Keck School of Medicine of USC; and John Kopchick of Ohio University were co-authors of the study.
Watch to this documentaire to Know how powerful nature really is…
Have you ever wondered how cannabinoids interact with your body? The answer is through the endocannabinoid system.
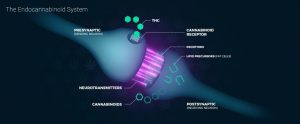
The endocannabinoid system is responsible for regulating balance in our body’s immune response, communication between cells, appetite and metabolism, memory, and more. 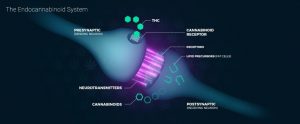 In spite of the integral role this system takes on, until recently it remained an unknown part of the human body’s functions.
In spite of the integral role this system takes on, until recently it remained an unknown part of the human body’s functions.
Named for the plant that inspired its discovery, the endocannabinoid system is important to your overall health and equilibrium, but its importance is only just becoming understood by the medical community. It is through this system that the naturally occurring cannabinoids from medical marijuana interact with our bodies and trigger its beneficial effects. With the potential to greatly affect the way our bodies work, a healthy endocannabinoid system is essential and it’s key that we recognize how to maintain it.
Across cultures and building through the 19th century, extractions of the cannabis plant were widely used for a number of medicinal purposes. However, following practical prohibition of the cannabis plant in 1937 by the U.S. government  for fear of abuse of its psychoactive properties, the medical use, experimentation, and study of cannabis were eliminated, stalling the progress of our understanding of the endocannabinoid system and the possible medical effects of cannabis. For nearly 50 years, marijuana fell from popular pharmacopeia and was labelled as illicit in the minds of Americans.
for fear of abuse of its psychoactive properties, the medical use, experimentation, and study of cannabis were eliminated, stalling the progress of our understanding of the endocannabinoid system and the possible medical effects of cannabis. For nearly 50 years, marijuana fell from popular pharmacopeia and was labelled as illicit in the minds of Americans.
Then the endocannabinoid system was defined in the early 1990’s when Lisa Matsuda announced that her team at the National Institute of Mental Health had first identified a THC-sensitive receptor in lab rat brains.
The path to the discovery of the endocannabinoid system, however, started more than a century earlier.
In 1895, researchers T. Barlow Wood, W.T. Newton Spivey, and Thomas Hill Easterfield became the first to isolate and identify a cannabis-derived cannabinoid, cannabinol (CBN) (Wood, Spivey & Easterfield, 1896). Over the next 70 years, researchers identified more cannabinoids, including R. Adams and others who identified and isolated CBD in 1940, and in 1964, Ralph Mechoulam and colleagues isolated and identified tetrahydrocannabinol (THC) (Pertwee, 2006) (Gaoni & Mechoulam, 1964). Following those monumental breakthroughs, researchers spent decades exploring those cannabinoids and their properties.
Before Matsuda’s discovery of the cannabinoid receptor in the animal’s brain, however, it was often speculated that cannabinoids produced their balancing effects via nonspecific interactions. Following this revelation, the National Academy of Science predicted the 1990s would be the “Decade of the Brain”. It turned out to be true as the following 10 year period would produce “more advances in neuroscience than in all previous years combined” (Lee, 2012).
It was in the early and mid-1990s Mechoulam and colleagues officially discovered the endocannabinoid system. It happened after he and his team were able to locate and identify two of the body’s naturally produced major endocannabinoids, anandamide and 2-arachidonoylglycerol, or 2-AG (Mechoulam & Hanus, 2000).
Since then, scientists have labored to learn as much as they can about the endocannabinoid system, our naturally occurring cannabinoids, and the ways cannabis alters this balance, publishing over 20,000 scientific studies referencing cannabinoids in just the last two decades.
The endocannabinoid system is made up of several integrated mechanisms:
These mechanisms are predominantly responsible for communication within the body to best regulate various biological responses.
One of the prime questions raised in these early studies was whether or not the body produces its own natural equivalents to the previously discovered compounds called phytocannabinoids, like THC and CBD, found in the cannabis plant (Mandal, 2014). The answer turned out to be “yes” – in the form of the endocannabinoids anandamide and 2-AG, which are like the two prominent analogs to THC and CBD, (Pacher et al, 2006). With the understanding that we humans create our own cannabinoids, the door to deconstructing their purpose was opened.
Endocannabinoids are created in response to needs within the larger physiological system and are largely understood to be used for the body’s regulatory functions. Acting backwards on presynaptic cells, they control the volume at which communicating signals are sent. It is in this way that endocannabinoids affect duration and intensity of the wide range of physiological processes under their control.
However, it has been repeatedly noted that, while the endocannabinoid system is linked to a number of important processes and is concentrated in the brain, nervous system, and reproductive organs, it does not affect regions of the brain controlling heart and lung function. This is one of the main reasons that fatal overdoses of cannabinoids do not occur (NCI, 2016).
Whenever there are deviations from homeostasis in the body’s functions, the endocannabinoid system is activated and begins to respond accordingly by synthesizing endocannabinoids, which act as neurotransmitters.
When the body creates neurotransmitters for the endocannabinoid system, they are picked up by specialized cannabinoid receptors, which sit on the surface of cells. These receptors are found in a wide range of physiological regions, such as in:
Like a key fits into a lock, endocannabinoids interact with these receptors and transmit information about changing conditions to kick-start a response, with the goal of helping the body achieve homeostasis, or equilibrium, within the body despite outside influences (Alger, 2013).
The endocannabinoid system’s receptor sites include CB1 and CB2 receptor variants, which respond differently to various cannabinoids (Pacher et al, 2006). CB1 receptors are most prevalent in the central nervous system and are linked to the following benefits:
CB2 receptors are found mostly on cells in the immune system and seem to dominate in fighting inflammation and damage to tissue. Some cells can even contain both types of receptors, each responsible for a different function.
There are two major endocannabinoids – 2-arachidonoylglycerol (2-AG) and Anandamide (AEA).
2-AG is considered a full agonist of both CB1 and CB2 receptors. This means that it binds with, and fits well inside, both receptors to activate them to stimulate a physiological response.
Anandamide is considered a partial agonist of both receptors, because, while it binds with and activates the receptors, it doesn’t fit as well inside them and subsequently doesn’t trigger such a powerful physiological response (Parcher, Batkai & Kunos, 2006).
Once the function that had deviated from homeostasis returns to equilibrium and the endocannabinoids are no longer needed, the third piece of the system – the metabolic enzymes – breaks down and degrades them.
Fatty acid amide hydrolase (FAAH) degrades Anandamide, and monoacylglycerol lipase (MAGL) breaks down 2-AG. By eliminating the endocannabinoids, the endocannabinoid system “turns off” the molecular signals and ends whatever physiological activity it had stimulated.
Since discovering the endocannabinoid system and its parts, researchers have worked to further understand how the endocannabinoid system may be used therapeutically to:
Overall, research indicates that the endocannabinoid system helps ensure that the body’s immune and central nervous systems are running correctly. Finding ways to modulate the endocannabinoid system’s activity opens pathways to an amazingly disparate set of chronic diseases and disorders (Pacher and Kunos, 2013).
For example, evidence indicates that stimulation of cannabinoid receptors may aid in the deletion of old traumatic memories and provide clinical benefits in age-related diseases associated with brain inflammation (Ruehle et al, 2012) (Marchalant, et al., 2008). This list also includes difficult conditions like Parkinson’s, multiple sclerosis, and cancer.
Memory
There is also evidence that the endocannabinoid system may aid in the deletion of old memories (Ruehle et al, 2012). The extinction of aversive memories is important to the progress of PTSD patients and in behavior conditioning for those with chronic anxiety. By allowing patients to forget painful memories, they can reset their stress and anxiety responses to certain experiences and substitute a more positive reaction.
Appetite & Weight
Cannabis has a well-known ability to increase appetite. However, because endocannabinoids are used internally for appetite control, inverse agonists to the CB1 receptor can be used to combat obesity by shutting off the body’s desire for food (Pagotto et al, 2005). The opposite can be accomplished by stimulating appetite in those suffering from wasting syndrome and allowing them to gain weight (Kogan and Mechoulam, 2007).
Finally, endocannabinoids also regulate metabolism and help control the transfer of energy through cells, ensuring optimal use of the food we do take in.
In today’s world, it is a common reality that the natural cycle of anxiety and physical response cannot be shut off due to constant exposure to stressors. Because cannabinoids affect the body’s glandular response to continued stress to regulate and temper response, the endocannabinoid system has implications for the way in which modern humans process long term stress and other enduring anxiety triggers (Akirav).
Immune Function & Inflammation
Additionally, endocannabinoids promote proper immune function to allow for a greater overall wellness. The role they play in immune homeostasis prevents “spontaneous activation of immune cell function”, helping to prevent inflammation and possibly even resulting neurological diseases (Pandey et al, 2009).
As scientists learn more about the endocannabinoid system, they also explore the potential role the cannabis-derived cannabinoids like THC, cannabidiol (CBD), cannabinol (CBN), and more could play in supporting the system.
Cannabinoids mimic the behavior of endocannabinoids and interact with the cannabinoid receptors to augment the endocannabinoid system. As the cannabinoids interact with the cannabinoid receptors, they stimulate various physiological responses.
THC, the well-recognized psychoactive compound found in medical marijuana, activates receptors to elicit a chemical response. It is considered an agonist of both CB1 and CB2 receptors because it directly binds to the receptors and activates them. THC tends to favor CB1 receptors because it fits very well inside them and therefore is able to stimulate a strong physiological reaction.
When THC reacts with CB1 receptors, this is what causes the well-known “high” feeling from marijuana. THC also directly activates CB2 receptors, but is considered a partial agonist and therefore doesn’t elicit such a strong physiological response.
CBD causes chemical changes by blocking receptors. It tends to have low affinity for both CB1 and CB2 receptors, and instead acts as an indirect antagonist of agonists. This means that CBD sits imperfectly inside the receptors, not activating them but preventing other chemical messengers like THC from binding to them (Pacher, Batkai & Kunos, 2006).
As we continue to learn more about the endocannabinoid system, we will also learn about the potential for the scope of active compounds from cannabis (like THC, CBD, and CBN) to be used therapeutically.
One theory about how the endocannabinoid system relates to our overall health is the proposed endocannabinoid deficiency syndrome, or CECD, which speculates that. for some people, the body does not generate enough endocannabinoids (Smith and Wagner, 2014). This concept, originally proposed by researcher E.B. Russo in 2004, further speculates that the deficiency could be the root cause of many autoimmune disorders, including migraines, fibromyalgia, and IBS (Russo, 2004).
By modulating the endocannabinoid system (Kaur, Ambwani & Singh, 2016), several diseases and conditions could possibly be treated, including:
One of the main obstacles to the acceptance and use of cannabis and its active cannabinoids in medicine is the problem of abuse for its psychoactivity. However, this issue does not arise in a number of possible approaches to the regulation of the endocannabinoid system:
Phytocannabinoids, like the THC from cannabis or the concentrated CBD in hemp, obviously affect the endocannabinoid system. However, it has also been shown that non-psychoactive phytocannabinoids from other plants, and even other compounds like terpenes and flavonoids, are picked up by receptors in our endocannabinoid systems (Gertsch et al, 2010).
Because small doses of phytocannabinoids can encourage the body to create more naturally occurring endocannabinoids and their receptors, it may be possible to bolster the sensitivity of our native systems with regular cannabinoid supplements (Pacher et al, 2006).
Overall, significant research must still be done to better understand the impact of the endocannabinoid system on our overall health and how supplementing our natural endocannabinoid production with plant-based cannabinoids may play a significant therapeutic role in our health. However, extensive early studies show great potential for using this vital system to the benefit of patient health.
To learn more about how individual cannabinoids can be used to promote overall well-being, read our informational articles on CBD, THC, CBN, and CBC, or visit our extensive collection of researchinto the conditions affected by cannabinoids and the endocannabinoid system.
example of the receptors..,
[1][2] a form of alternative medicine, aims to maintain human health through nutritional supplementation. The concept builds on the idea of an optimum nutritional environment in the body and suggests that diseases reflect deficiencies in this environment. Treatment for disease, according to this view, involves attempts to correct “imbalances or deficiencies based on individual biochemistry” by use of substances such as vitamins, minerals, amino acids, trace elements and fatty acids.[3][4][5] The notions behind orthomolecular medicine are not supported by sound medical evidence and the therapy is not effective;[6][7] even the validity of calling the orthomolecular approach a form of medicine has been questioned since the 1970s.[8]
The approach is sometimes referred to as megavitamin therapy[1][2] because its practice evolved out of, and in some cases still uses, doses of vitamins and minerals many times higher than the recommended dietary intake. Orthomolecular practitioners may also incorporate a variety of other styles of treatment into their approaches, including dietary restriction, megadoses of non-vitamin nutrients and mainstream pharmaceutical drugs.[1][9] Proponents argue that non-optimal levels of certain substances can cause health issues beyond simple vitamin deficiency and see balancing these substances as an integral part of health.[10]
Linus Pauling coined the term “orthomolecular” in the 1960s to mean “the right molecules in the right amounts” (ortho- in Greek implies “correct”).[11] Proponents of orthomolecular medicine hold that treatment must be based on each patient’s individual biochemistry.[12][13]
The scientific and medical consensus holds that the broad claims of efficacy advanced by advocates of orthomolecular medicine are not adequately tested as drug therapies.[6] It has been described as a form of food faddism and as quackery.[14] Proponents point to mainstream sources that have published research supporting the benefits of nutrient supplementation[15][16] and to instances where conventional medicine uses vitamins as treatments for some diseases.
Some vitamins in large doses have been linked to increased risk of cardiovascular disease, of cancer and of death.[17][18][19] The scientific consensus view is that for normal individuals, a balanced diet contains all necessary vitamins and minerals, and that routine supplementation is not necessary absent specific diagnosed deficiencies.[20]
In the early 20th century, some doctors hypothesised that vitamins could cure disease, and supplements were prescribed in megadoses by the 1930s.[21] Their effects on health were disappointing, though, and in the 1950s and 1960s, nutrition was de-emphasised in standard medical curricula.[21] Riordon’s organization cite figures from this period as founders of their movement,[22] although the word “orthomolecular” was coined by Linus Pauling only in 1967.
Amongst the individuals described posthumously as orthomolecularists are Max Gerson, who developed a diet that he claimed could treat diseases, which the American Medical Association’s 1949 Council on Pharmacy and Chemistry found ineffective;[23] and the Shute brothers, who attempted to treat heart disease with vitamin E.[24] Several concepts now cited by orthomolecularists, including individual biochemical variation[13] and inborn errors of metabolism,[21][25][26] debuted in scientific papers early in the 20th century.
In 1948, William McCormick theorized that vitamin C deficiency played an important role in many diseases and began to use large doses in patients.[27] In the 1950s, Fred R. Klenner also tried vitamin C megadosage as a therapy for a wide range of illnesses, including polio.[28] Irwin Stone stated that organisms that do not synthesise their own vitamin C due to a loss-of-function mutation have a disease he called “hypoascorbemia”.[29] This term is not used by the medical community, and the idea of an organism-wide lack of a biosynthetic pathway as a disease was not endorsed by Stone’s contemporaries.[30]
In the 1950s, some individuals believed that vitamin deficiencies caused mental illness.[21] Psychiatrists Humphry Osmond and Abram Hoffer gave people having acute schizophrenic episodes high doses of niacin,[31] while William Kaufman used niacinamide. While niacin has no known efficacy in psychiatric disease, the use of niacin in combination with statins and other medical therapies has become one of several medical treatments for cardiovascular disease.[32][33]
In the late 1960s, Linus Pauling introduced the expression “orthomolecular”[11] to express the idea of the right molecules in the right amounts.[11] Since the first claims of medical breakthroughs with vitamin C by Pauling and others, findings on the health effects of vitamin C have been controversial and contradictory.[34][35] Pauling’s claims have been criticised as overbroad.[36]
Later research branched out into nutrients besides niacin and vitamin C, including essential fatty acids.[37]
According to Abram Hoffer, orthomolecular medicine does not purport to treat all diseases, nor is it “a replacement for standard treatment. A proportion of patients will require orthodox treatment, a proportion will do much better on orthomolecular treatment, and the rest will need a skillful blend of both.”[38] Nevertheless, advocates have said that nutrients can prevent,[39] treat, and sometimes cure a wide range of medical conditions, including: acne,[40] alcoholism,[41] allergies, arthritis, autism, bee stings, bipolar disorder, burns, cancer,[42][43] the common cold, depression, drug addiction, drug overdose, epilepsy, heart diseases, heavy metal toxicity, acute hepatitis, herpes, hyperactivity, hypertension, hypoglycemia, influenza, learning disabilities, mental and metabolic disorders,[44] migraine, mononucleosis, mushroom poisoning, neuropathy & polyneuritis (including multiple sclerosis), osteoporosis,[45] polio, an hypothesised condition called “pyroluria”, radiation sickness, Raynaud’s disease, mental retardation, schizophrenia,[4] shock, skin problems, snakebite, spider bite, tetanus toxin and viral pneumonia.[46]
Hoffer believed that particular nutrients could cure mental illness. In the 1950s, he attempted to treat schizophrenia with niacin, although proponents of orthomolecular psychiatry say that the ideas behind their approach predate Hoffer.[47][48] According to Hoffer and others who called themselves “orthomolecular psychiatrists”, psychiatric syndromes result from biochemical deficiencies, allergies, toxicities or several hypothetical contributing conditions which they termed pyroluria, histadelia and histapenia. These purported causes were said to be found during an “individual biochemical workup” and treated with megavitamin therapy and dietary changes including fasting.[49] These diagnoses and treatments are not accepted by evidence-based medicine.[50]
According to Abram Hoffer, “primitive” peoples do not consume processed foods and do not have “degenerative” diseases.[51] In contrast, typical “Western” diets are said to be insufficient for long-term health, necessitating the use of megadose supplements of vitamins, dietary minerals, proteins, antioxidants, amino acids, ω-3 fatty acids, ω-6 fatty acids, medium-chain triglycerides, dietary fiber, short and long chain fatty acids, lipotropes, systemic and digestive enzymes, other digestive factors, and prohormones to ward off hypothetical metabolism anomalies at an early stage, before they cause disease.[38]
Orthomolecularists say that they provide prescriptions for optimal amounts of micronutrients after individual diagnoses based on blood tests and personal histories.[3][12] Lifestyle and diet changes may also be recommended. The battery of tests ordered includes many that are not considered useful by medicine.[50]
Orthomolecular medicine is practiced by few medical practitioners.[52][53]
A survey released in May, 2004 by the National Center for Complementary and Alternative Medicine focused on who used alternative medicine, what was used, and why it was used in the United States by adults age 18 years and over during 2003. The survey reported uses in the previous twelve months that include orthomolecular related uses: Nonvitamin, nonmineral, natural products 18.9%, Diet-based therapies 3.5%, Megavitamin therapy 2.8%.[54]
Another recent CAM survey reported that 12% of liver disease patients used the antioxidant silymarin, more than 6% used vitamins, and that “in all, 74% of patients reported using CAM in addition to the medications prescribed by their physician, but 26% did not inform their physician of their CAM use.”[55]
Even though the health benefits are not established, the use of high doses of vitamins is also common in people who have been diagnosed with cancer.[56] According to Cancer Research UK, cancer patients should always seek professional advice before taking such supplements, and using them as a substitute for conventional treatment “could be harmful to [their] health and greatly reduce the chance of curing or controlling [their] cancer”.[57]
Orthomolecular therapies have been criticized as lacking a sufficient evidence base for clinical use: their scientific foundations are too weak, the studies that have been performed are too few and too open to interpretation, and reported positive findings in observational studies are contradicted by the results of more rigorous clinical trials.[52][58] Accordingly, “there is no evidence that orthomolecular medicine is effective”. Proponents of orthomolecular medicine strongly dispute this statement by citing studies demonstrating the effectiveness of treatments involving vitamins, though this ignores the belief that a normal diet will provide adequate nutrients to avoid deficiencies, and that orthomolecular treatments are not actually related to vitamin deficiency.[10] The lack of scientifically rigorous testing of orthomolecular medicine has led to its practices being classed with other forms of alternative medicine and regarded as unscientific.[59][60][61] It has been described as food faddism and quackery, with critics arguing that it is based upon an “exaggerated belief in the effects of nutrition upon health and disease.”[62][63][64] Orthomolecular practitioners will often use dubious diagnostic methods to define what substances are “correct”; one example is hair analysis, which produces spurious results when used in this fashion.[10]
Proponents of orthomolecular medicine contend that, unlike some other forms of alternative medicine such as homeopathy, their ideas are at least biologically based, do not involve magical thinking,[65] and are capable of generating testable hypotheses.[66] Orthomolecular is not a standard medical term, and clinical use of specific nutrients is considered a form of chemoprevention (to prevent or delay development of disease) or chemotherapy (to treat an existing condition).[67]
Despite a lack of evidence for its efficacy, interest in intravenous high dose vitamin C therapy has not been permanently extinguished, and some research groups continue to investigate whether it has an effect as a possible cancer treatment.[68][69]
In general, the vitamin megadoses advocated by orthomolecular medicine are unsupported by scientific consensus.[32] Some vitamins are toxic in high doses,[70] including niacin (B3),[71]cholecalciferol (D)[72] and tocopherol (E).[73] The view of the medical community is that there is no evidence for the efficacy of Orthomolecular medicine as a treatment for cancer,[6] and that high vitamin doses may – on the contrary – increase overall mortality.[74] Nutritional treatments are not generally accepted as being helpful for psychological health.[75] Its claims have been criticized by most medical organizations, including the American Cancer Society, the American Psychiatric Association, the National Institute of Mental Health,[50] the American Academy of Pediatrics,[76]CHAMPUS, and the Canadian Paediatric Society. The American Medical Association describes as “myths” the ideas that adequate nutrition is not readily achievable with normal food, all food grown with pesticide is poisonous, all food additives are poisonous, vitamin and mineral deficiencies are common, that the cause of most disease is poor diet, which can be prevented by nutritional supplements. [77]
Similarly, the American Cancer Society comments that the current scientific evidence does not “support use of orthomolecular therapy for most of the conditions for which it is promoted.” Some supplements have exhibited benefits for specific conditions, while a few have been confirmed to be harmful; the consumption of nutritious foods is the best recognized method to obtain vitamins, minerals, and nutrients crucial for good health.[32] Barrie Cassileth, an adviser on alternative medicine to the National Institutes of Health, stated that “scientific research has found no benefit from orthomolecular therapy for any disease,”[52] and medical textbooks also report that there is “no evidence that megavitamin or orthomolecular therapy is effective in treating any disease.”[78]
A 1973 task force of the American Psychiatric Association unanimously concluded:
This review and critique has carefully examined the literature produced by megavitamin proponents and by those who have attempted to replicate their basic and clinical work. It concludes in this regard that the credibility of the megavitamin proponents is low. Their credibility is further diminished by a consistent refusal over the past decade to perform controlled experiments and to report their new results in a scientifically acceptable fashion. Under these circumstances this Task Force considers the massive publicity which they promulgate via radio, the lay press and popular books, using catch phrases which are really misnomers like “megavitamin therapy” and “orthomolecular treatment,” to be deplorable.[79]
In response to claims that orthomolecular medicine could cure childhood psychoses and learning disorders, the American Academy of Pediatrics labelled orthomolecular medicine a “cult” in 1976.[80]
Proponents of orthomolecular medicine counter that some vitamins and nutrients are now used in medicine as treatments for specific diseases, such as megadose niacin and fish oil for dyslipidemias, and megavitamin therapies for a group of rare inborn errors of metabolism.[21] A review in the Annals of Internal Medicine concluded that while some therapies might be beneficial, others might be harmful or interfere with effective medical therapy.[81] A recent study of over 161,000 individuals provided, in the words of the authors, “convincing evidence that multivitamin use has little or no influence on the risk of common cancers, cardiovascular disease, or total mortality in postmenopausal women.”[82] A recent meta-analysis in JAMA suggested that supplementation with combinations of antioxidant vitamins (beta-carotene, vitamin A, and vitamin E) may increase mortality, although with respect to beta-carotene this conclusion may be due to the known harmful effect in smokers.[83]
In the United States, pharmaceuticals must be proven safe and effective to the satisfaction of the FDA before they can be marketed, whereas dietary supplements must be proven unsafe before regulatory action can be taken.[84] A number of orthomolecular supplements are available in the US in pharmaceutical versions that are sometimes quite similar in strength and general content, or in other countries are regulated as pharmaceuticals. The US regulations also have provisions to recognize a general level of safety for established nutrients that can forgo new drug safety tests. Proponents of orthomolecular medicine argue that supplements are less likely to cause dangerous side-effects or harm, since they are normally present in the body.[5] Some vitamins are toxic in high doses[70] and nearly all (with the possible exception of Vitamin C[85]) will cause adverse effects given high levels of overdosing for prolonged periods as recommended by orthomolecular practitioners.[10] Forgoing medical care in favor of orthomolecular treatments can lead to adverse health outcomes.[6]
Health professionals see orthomolecular medicine as encouraging individuals to dose themselves with large amounts of vitamins and other nutrients without conventional supervision, which they worry might be damaging to health. Potential risks[86] of inappropriate vitamin and supplement regimes include an increased risk of coronary heart disease,[87] hypertension, thrombophlebitis, peripheral neuropathy, ataxia, neurological effects, liver toxicity, congenital abnormalities, spontaneous abortion, gouty arthritis, jaundice, kidney stones, and diarrhea.[7][17][88][89][90][91][92] In their book Trick or Treatment?, Edzard Ernst and Simon Singh conclude that “The concepts of orthomolecular medicine are not biologically plausible and not supported by the results of rigorous clinical trials. These problems are compounded by the fact that orthomolecular medicine can cause harm and is often very expensive.”[10]
Orthomolecular proponents claim that even large doses of vitamin E pose no risk to health and are useful for the treatment and prevention of a broad list of conditions, including heart and circulatory diseases, diabetes and nephritis.[93] Initial hopes for the usefulness of vitamin E in orthomolecular medicine were based on epidemiological studies suggesting that people who consumed more vitamin E had lower risks of chronic disease, such as coronary heart disease.[94] These observational studies could not distinguish between whether the higher levels of vitamin E improved health themselves, or whether confounding variables (such as other dietary factors or exercise) were responsible.[95][96] To distinguish between these possibilities, a number of randomized controlled trials were performed and meta-analysis of these controlled clinical trials have not shown any clear benefit from any form of vitamin E supplementation for preventing chronic disease.[97][98][99][100] Further clinical studies show no benefit of vitamin E supplements for cardiovascular disease.[101] The current position of the American National Institutes of Healthis that there is no convincing evidence that vitamin E supplements can prevent or treat any disease.[102]
Beyond the lack of apparent benefit, a series of three meta-analyses reported that vitamin E supplementation is associated with an increased risk of death; one of the meta-analyses performed by the Cochrane Collaboration also found significantly increased mortality for the antioxidant vitamins A and beta-carotene.[103][104][105] A subsequent meta-analysis found no mortality benefit from vitamin E, but also no increase in mortality either.[106]
Several articles in the alternative-medicine literature have suggested that orthomolecular-related dietary supplementation might be helpful for patients with HIV/AIDS.[107][108] A study using 250 mg and 1000 mg doses of vitamin C along with other antioxidants to treat people with AIDS did not find any benefit.[109] However, these doses are far smaller than the ones used by orthomolecular physicians for treatment of AIDS.[110][unreliable medical source?]
A meta analysis in 2010 found that micronutrient supplementation decreased the risk of death and improved outcomes in pregnant women with HIV in Africa.[111] A 2017 Cochrane review found no strong evidence to suggest that micronutrient supplementation prevents death or is effective at slowing the progression of disease for adults with HIV.[112] It is important for people living HIV to eat a healthy adequate diet.[112] For people with HIV that have clinically demonstrated deficiencies in micronutrients or for people who are not able to consume the recommended daily quantities of minerals and vitamins, supplementation is still encouraged.[112] Vitamin A in children with HIV appears to be safe and beneficial.[113] Vitamin A deficiency is found in children with HIV infection who may or may not have symptoms of AIDS. Vitamin A supplementation reduces morbidity and mortality in AIDS symptomatic children, but has no effect on asymptomatic children. It does not prevent HIV infection, cannot treat the chronic HIV infection, and will not cure AIDS.[114][115]
Matthias Rath has been extensively criticized for presenting his vitamin supplements as a treatment for AIDS and for testing them in illegal trials in South Africa.[116][117] A former associate of Linus Pauling, Rath has promoted vitamins as a treatment for HIV infection, describing treatment with effective antiretroviral drugs as toxic and part of a global conspiracy serving the financial interests of the pharmaceutical industry.[118] In a lawsuit that found against Rath, the South African Medical Association blamed his vitamin products for several deaths.[117][119][120] The World Health Organization and two health agencies of the United Nations also described Rath’s advertisements as “wrong and misleading” and “an irresponsible attack on ARV (antiretroviral) therapy.”[121] The South African Centre for Social Science Research described the trials as “state sponsored pseudo-science”.[122] Rath’s trials, conducted with the aid of AIDS denialist David Rasnick, were declared unlawful by the Cape High Court; Rath, Rasnick and their foundation were barred from conducting further unauthorised clinical trials and from advertising their products.[123]
Advocates of orthomolecular medicine, including Pauling, Hoffer and Ewan Cameron have claimed that their findings are actively suppressed by the medical and pharmaceutical industry. Hoffer wrote “There is no conspiracy led and directed by a single person or by a single organization. There is no Mafia in psychiatry. However, there is a conspiracy led and directed by a large number of professionals and their associations who have a common aim to protect their hard-earned orthodoxy, no matter what the cost to their opponent colleagues or to their patients.”.[124][125]
The Journal of Orthomolecular Medicine, founded in 1967 as the Journal of Schizophrenia, is a major publication of orthomolecular medicine. As Abram Hoffer wrote:
Other members of the medical community deny the existence of such an institutional prejudice.[127][128] A review in the Journal of Clinical Oncology denied that physicians collude against unconventional treatments.[129] Despite claims of conspiracy, the Linus Pauling Institute‘s funding comes primarily from the National Institutes of Health,[130] and in 1995 some orthomolecular therapies were reported as being sanctioned in Japan.[131]
This review looks at the role of an alkaline diet in health. Pubmed was searched looking for articles on pH, potential renal acid loads, bone health, muscle, growth hormone, back pain, vitamin D and chemotherapy. Many books written in the lay literature on the alkaline diet were also reviewed and evaluated in light of the published medical literature. There may be some value in considering an alkaline diet in reducing morbidity and mortality from chronic diseases and further studies are warranted in this area of medicine.
Life on earth depends on appropriate pH levels in and around living organisms and cells. Human life requires a tightly controlled pH level in the serum of about 7.4 (a slightly alkaline range of 7.35 to 7.45) to survive [1].
As a comparison, in the past 100 years with increasing industrialization, the pH of the ocean has dropped from 8.2 to 8.1 because of increasing CO2 deposition. This has a negative impact on life in the ocean [1, 2] and may lead to the collapse of the coral reefs [3]. Even the pH of the soil in which plants are grown can have considerable influence on the mineral content of the food we eat (as minerals are used as buffers to maintain pH). The ideal pH of soil for the best overall availability of essential nutrients is between 6 and 7. Acidic soils below pH of 6 may have reduced calcium and magnesium, and soil above pH 7 may result in chemically unavailable iron, manganese, copper and zinc. Adding dolomite and manure are ways of raising pH in an acid soil environment when the pH is below 6 .
When it comes to the pH and net acid load in the human diet, there has been considerable change from the hunter gather civilization to the present [5]. With the agricultural revolution (last 10,000 years) and even more recently with industrialization (last 200 years), there has been an decrease in potassium (K) compared to sodium (Na) and an increase in chloride compared to bicarbonate found in the diet. The ratio of potassium to sodium has reversed, K/Na previously was 10 to 1 whereas the modern diet has a ratio of 1 to 3 [7]. It is generally accepted that agricultural humans today have a diet poor in magnesium and potassium as well as fiber and rich in saturated fat, simple sugars, sodium, and chloride as compared to the preagricultural period [6]. This results in a diet that may induce metabolic acidosis which is mismatched to the genetically determined nutritional requirements [8]. With aging, there is a gradual loss of renal acid-base regulatory function and a resultant increase in diet-induced metabolic acidosis while on the modern diet [9]. A low-carbohydrate high-protein diet with its increased acid load results in very little change in blood chemistry, and pH, but results in many changes in urinary chemistry. Urinary magnesium levels, urinary citrate and pH are decreased, urinary calcium, undissociated uric acid, and phosphate are increased. All of these result in an increased risk for kidney stones [10].
Much has been written in the lay literature as well as many online sites expounding on the benefits of the alkaline diet. This paper is an attempt to balance the evidence that is found in the scientific literature.
The pH in our body may vary considerably from one area to another with the highest acidity in the stomach (pH of 1.35 to 3.5) to aid in digestion and protect against opportunistic microbial organisms. But even in the stomach, the layer just outside the epithelium is quite basic to prevent mucosal injury. It has been suggested that decreased gastric lining secretion of bicarbonates and a decrease in the alkaline/acid secretion in duodenal ulcer patients may play a significant role in duodenal ulcers [11]. The skin is quite acidic (pH 4–6.5) to provide an acid mantle as a protective barrier to the environment against microbial overgrowth. There is a gradient from the outer horny layer (pH 4) to the basal layer (pH 6.9) [12]. This is also seen in the vagina where a pH of less than 4.7 protects against microbial overgrowth [13].
The urine may have a variable pH from acid to alkaline depending on the need for balancing the internal environment. Acid excretion in the urine can be estimated by a formula described by Remer (sulfate + chloride + 1.8x phosphate + organic acids) minus (sodium + potassium + 2x calcium + 2x magnesium) mEq [14]. Foods can be categorized by the potential renal acid loads (PRALs) see Table 2. Fruits, vegetables, fruit juices, potatoes, and alkali-rich and low phosphorus beverages (red and white wine, mineral soda waters) having a negative acid load. Whereas, grain products, meats, dairy products, fish, and alkali poor and low phosphorus beverages (e.g., pale beers, cocoa) have relatively high acid loads [15]. Measurement of pH of the urine (reviewed in a recent study with two morning specimens done over a five-year span) did not predict bone fractures or loss of bone mineral density [16]. However, this may not be reflective of being on an alkaline or acid diet throughout this time. For more details, see Table 1.
Calcium in the form of phosphates and carbonates represents a large reservoir of base in our body. In response to an acid load such as the modern diet these salts are released into the systemic circulation to bring about pH homeostasis [7]. It has been estimated that the quantity of calcium lost in the urine with the modern diet over time could be as high as almost 480 gm over 20 years or almost half the skeletal mass of calcium [21]. However, urinary losses of calcium are not a direct measure of osteoporosis. There are many regulatory factors that may compensate for the urinary calcium loss. When the arterial pH is in the normal range, a mild reduction of plasma bicarbonate results in a negative calcium balance which could benefit from supplementing bicarbonate in the form of potassium bicarbonate [22]. It has been found that bicarbonate, which increases the alkali content of a diet, but not potassium may attenuate bone loss in healthy older adults [23]. The bone minerals that are wasted in the urine may not have complete compensation through intestinal absorption, which is thought to result in osteoporosis. However, adequate vitamin D with a 25(OH)D level of >80 nmol/L may allow for appropriate intestinal absorption of calcium and magnesium and phosphate when needed [24]. Sadly, most populations are generally deficient in vitamin D especially in northern climates [25]. In chronic renal failure, correction of metabolic acidosis with bicarbonate significantly improves parathyroid levels and levels of the active form of vitamin D 1,25(OH)2D3 [26]. Recently, a study has shown the importance of phosphate in Remer’s PRAL formula. According to the formula it would be expected that an increase in phosphate should result in an increase in urinary calcium loss and a negative calcium balance in bone [27]. It should be noted that supplementation with phosphate in patients with bed rest reduced urinary calcium excretion but did not prevent bone loss [28]. The most recent systematic review and meta-analysis has shown that calcium balance is maintained and improved with phosphate which is quite contrary to the acid-ash hypothesis [29]. As well a recent study looking at soda intake (which has a significant amount of phosphate) and osteoporosis in postmenopausal American first nations women did not find a correlation [30]. It is quite possible that the high acid content according to Remer’s classification needs to be looked at again in light of compensatory phosphate intake. There is online information promoting an alkaline diet for bone health as well as a number of books. However, a recent systematic review of the literature looking for evidence supporting the alkaline diet for bone health found no protective role of dietary acid load in osteoporosis [31].
Another element of the modern diet is the excess of sodium in the diet. There is evidence that in healthy humans the increased sodium in the diet can predict the degree of hyperchloremic metabolic acidosis when consuming a net acid producing diet [32]. As well, there is evidence that there are adverse effects of sodium chloride in the aging population. A high sodium diet will exacerbate disuse-induced bone and muscle loss during immobilization by increasing bone resorption and protein wasting [33]. Excess dietary sodium has been shown to result in hypertension and osteoporosis in women [34, 35]. As well, dietary potassium which is lacking in the modern diet would modulate pressor and hypercalciuric effects of excess of sodium chloride [36].
Excess dietary protein with high acid renal load may decrease bone density if not buffered by ingestion of supplements or foods that are alkali rich [37]. However, adequate protein is necessary for prevention of osteoporosis and sarcopenia; therefore, increasing the amount of fruit and vegetables may be necessary rather than reducing protein [38].
As we age, there is a loss of muscle mass, which may predispose to falls and fractures. A three-year study looking at a diet rich in potassium, such as fruits and vegetables, as well as a reduced acid load, resulted in preservation of muscle mass in older men and women [39]. Conditions such as chronic renal failure that result in chronic metabolic acidosis result in accelerated breakdown in skeletal muscle [40]. Correction of acidosis may preserve muscle mass in conditions where muscle wasting is common such as diabetic ketosis, trauma, sepsis, chronic obstructive lung disease, and renal failure [41]. In situations that result in acute acidosis, supplementing younger patients with sodium bicarbonate prior to exhaustive exercise resulted in significantly less acidosis in the blood than those that were not supplemented with sodium bicarbonate [42].
It has long been known that severe forms of metabolic acidosis in children, such as renal tubular acidosis, are associated with low levels of growth hormone with resultant short stature. Correction of the acidosis with bicarbonate [7] or potassium citrate [43] increases growth hormone significantly and improved growth. The use of enough potassium bicarbonate in the diet to neutralize the daily net acid load in postmenopausal women resulted in a significant increase in growth hormone and resultant osteocalcin [44]. Improving growth hormone levels may improve quality of life, reduce cardiovascular risk factors, improve body composition, and even improve memory and cognition [45]. As well this results in a reduction of urinary calcium loss equivalent to 5% of bone calcium content over a period of 3 years [46].
There is some evidence that chronic low back pain improves with the supplementation of alkaline minerals [47]. With supplementation there was a slight but significant increase in blood pH and intracellular magnesium. Ensuring that there is enough intracellular magnesium allows for the proper function of enzyme systems and also allows for activation of vitamin D [48]. This in turn has been shown to improve back pain [49].
The effectiveness of chemotherapeutic agents is markedly influenced by pH. Numerous agents such as epirubicin and adriamycin require an alkaline media to be more effective. Others, such as cisplatin, mitomycin C, and thiotepa, are more cytotoxic in an acid media [50]. Cell death correlates with acidosis and intracellular pH shifts higher (more alkaline) after chemotherapy may reflect response to chemotherapy [51]. It has been suggested that inducing metabolic alkalosis may be useful in enhancing some treatment regimes by using sodium bicarbonate, carbicab, and furosemide [52]. Extracellular alkalinization by using bicarbonate may result in improvements in therapeutic effectiveness [53]. There is no scientific literature establishing the benefit of an alkaline diet for the prevention of cancer at this time.
The human body has an amazing ability to maintain a steady pH in the blood with the main compensatory mechanisms being renal and respiratory. Many of the membranes in our body require an acid pH to protect us and to help us digest food. It has been suggested that an alkaline diet may prevent a number of diseases and result in significant health benefits. Looking at the above discussion on bone health alone, certain aspects have doubtful benefit. There does not seem to be enough evidence that milk or cheese may be as detrimental as Remer’s formula suggests since phosphate does benefit bone health and result in a positive calcium balance. However, another mechanism for the alkaline diet to benefit bone health may be the increase in growth hormone and resultant increase in osteocalcin. There is some evidence that the K/Na ratio does matter and that the significant amount of salt in our diet is detrimental. Even some governments are demanding that the food industry reduce the salt load in our diet. High-protein diets may also affect bone health but some protein is also needed for good bone health. Muscle wasting however seems to be reduced with an alkaline diet and back pain may benefit from this as well. An alkaline environment may improve the efficacy of some chemotherapy agents but not others.
Alkaline diets result in a more alkaline urine pH and may result in reduced calcium in the urine, however, as seen in some recent reports, this may not reflect total calcium balance because of other buffers such as phosphate. There is no substantial evidence that this improves bone health or protects from osteoporosis. However, alkaline diets may result in a number of health benefits as outlined below
From the evidence outlined above, it would be prudent to consider an alkaline diet to reduce morbidity and mortality of chronic disease that are plaguing our aging population. One of the first considerations in an alkaline diet, which includes more fruits and vegetables, is to know what type of soil they were grown in since this may significantly influence the mineral content. At this time, there are limited scientific studies in this area, and many more studies are indicated in regards to muscle effects, growth hormone, and interaction with vitamin D.